Heartbroken Blackpool mum speaks out after six-week-old baby boy dies from meningitis
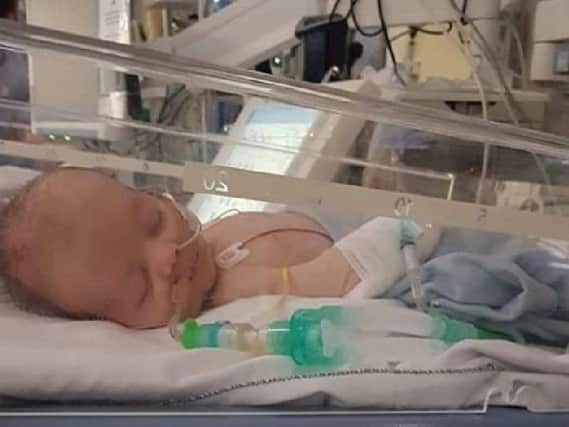

Georgia Higginbottom was faced with every parent’s worst nightmare when six-week-old Oscar Nally was struck down by meningitis.
Ahead of his funeral today, the 21-year-old courageously spoke of her son’s final moments in the hope other families will spot the deadly signs of the disease – and be able to prevent further tragedies.
Advertisement
Hide AdAdvertisement
Hide AdShe said: “He was really poorly and, if he had survived, all he would have been able to do is breathe, and that’s not a life.
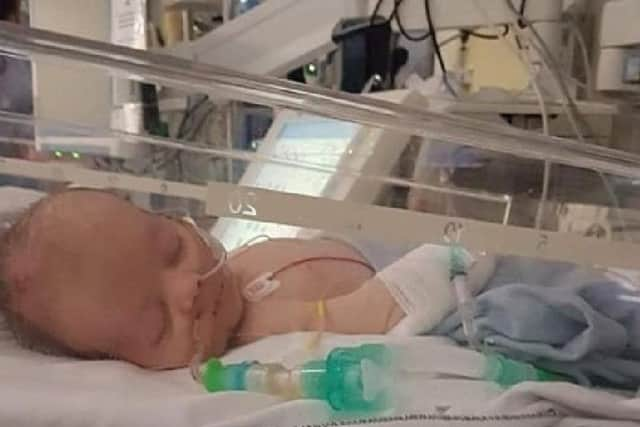

“I did not realise how serious this disease was.”
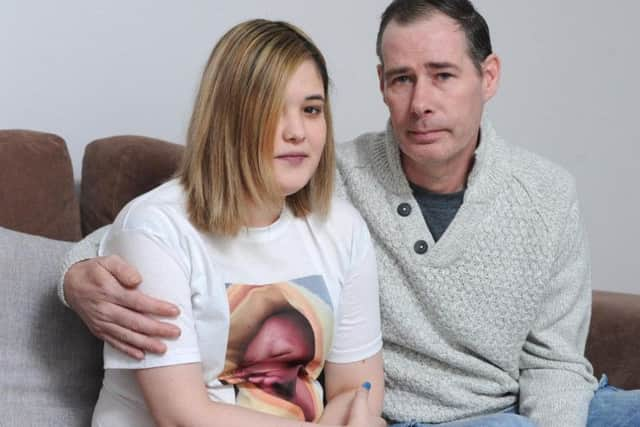
Georgia’s mum, Sharon Smith, 45, said: “He brought so much love into our house. Now that has been taken away.
“We just feel empty and numb. It’s horrible. A part of our hearts is gone.”
A month after being born two weeks early on Friday, September 28, Oscar was taken to Blackpool Victoria Hospital with a suspected infection after paramedics were called to his home in Stuart Place, Grange Park.

Advertisement
Hide AdAdvertisement
Hide AdHis condition improved after he was given antibiotics through a drip and, 48 hours later, he was allowed home.
He seemed “good in himself” and like “just a normal, typical baby”, Sharon said, but, two weeks later, on Friday, November 9, Oscar suddenly fell ill again.
“In the morning, I was playing with him,” Sharon said.
“Georgia fed him at noon. By 12.30pm he was in the Walk-In Centre fighting for his life.


“Within seconds of us putting him down, he woke up with a cry; a shrill cry. It was horrible.
Advertisement
Hide AdAdvertisement
Hide Ad“To look at him, you would not think there was anything wrong with him. We thought he had a bit too much milk to drink or something.”
The family went to the Walk-In Centre in Whitegate Drive – now called the Urgent Treatment Centre – when Oscar’s breathing became “wheezy”, Sharon said.
His temperature was 39.7C. A fever is usually considered to be a temperature of 38C or above.
A doctor gave Oscar oxygen before calling ahead to the hospital.
Advertisement
Hide AdAdvertisement
Hide AdSharon said: “When we got out of the ambulance, all these emergency staff were there, and they took him into this room.
“They helped him and they did their best, but they had to put him on life support and transfer him to Manchester.
“This was in the space of three hours.”
It was at the Royal Manchester Children’s Hospital that tests confirmed medics’ suspicions of Group B streptococcal meningitis (GBS), the main cause of meningitis in babies.
A brain scan was done, and a doctor took Oscar’s family into a side room to break the devastating news that the youngster would not survive his ordeal.
Advertisement
Hide AdAdvertisement
Hide Ad“I couldn’t go in the room when they were properly explaining what was wrong because I was so upset,” Georgia said.
“But then I held him and I knew he was not right.”
Sharon added: “They showed us the pictures. Every single part of his brain was black. Georgia had him in her arms and he was fitting.”
Oscar was hastily Christened and then, wrapped in his mother’s arms, his life support machine was shut down.
“It was a joint decision because Oscar had already gone up to the angels,” Sharon said. “He had already gone.
Advertisement
Hide AdAdvertisement
Hide Ad“Georgia held him in her arms from 2am until 10am when he passed away. She did not move.”
Oscar died on Tuesday, November 13. He was just 46 days old.
Since then, Georgia and her family have been staying with him in the Butterfly Suite at Brian House Children’s Hospice in Bispham.
There, in a Moses basket and surrounded by his teddy bears, he remained with his loved ones by his side before today’s final farewell, at Carleton Chapel and Cemetery at 9.30am.
Advertisement
Hide AdAdvertisement
Hide AdOscar did not have a rash when he fell ill and, according to the charity Meningitis Now, the signs of meningitis can be difficult to recognise in very young babies.
“If you think there’s something wrong with your child, get them seen,” Sharon urged.
“Even if it’s the tiniest thing. It’s just a mother’s instinct. We just want to try and help people.”
Grieving Georgia added: “It’s really, really important. I did not realise how serious this disease was.”
Advertisement
Hide AdAdvertisement
Hide AdSteve Dayman, who founded Meningitis Now after his son Spencer died in 1982, said: “There are different strains of bacterial meningitis.
“It’s a very difficult disease to diagnose and identify. In most cases you will notice a rapid deterioration.
“The key to all this is not to wait for a rash. Sometimes it can be a late symptom, and other times it might not appear at all.
“Even in the best hands in the big city hospitals, sometimes it’s still not enough to save that life.”
HOW IS GBS CAUSED?
Advertisement
Hide AdAdvertisement
Hide AdIt is usually caused by Streptococcus agalactiae bacteria, which tend to live harmlessly in the intestinal tract or vagina, according to Meningitis Now.
Very few adults develop it, but newborn babies don’t have a fully developed immune system, which allows the bacteria to spread through the blood and cause serious illness.
Tests carried out on Oscar during his first stay in hospital did not show any signs, Sharon said. “They said it can hide in the digestive system,” she added.
The risk of GBS is higher if:
++ The mother previously had a baby with GBS;
++ Swabs and urine samples from mum tested positive for it;
++ The mother had a high temperature during labour;
++ The baby is part of a multiple birth [ie twins or triplets];
++ It is born prematurely; or
Advertisement
Hide AdAdvertisement
Hide Ad++ The time between the waters breaking and the delivery of the baby is prolonged
WHAT ARE THE SYMPTOMS?
++Fever - sometimes with cold hands and feet
++A reluctance to feed
++ Vomiting and/or diarrhoea
++ Irritability
++ Floppiness, a difficulty to wake, or unresponsiveness
++ A difficulty breathing, or grunting
++ Faster or slower than normal breathing
++ Pale or blotchy skin
++ Red or purple spots or a rash that does not fade under pressure, such as a glass being applied
++ A high-pitched cry, moaning, or whimpering
++ A bulging soft spot
++ Convulsions or seizures
++ An arched back
++ A swollen abdomen
++ Dry nappies
Meningitis Now said: “The signs and symptoms of meningitis or septicaemia are often non-specific at first and can be difficult to recognise in very young babies.
“Trust your instincts as a parent or carer. Seek urgent medical attention if you suspect your child is ill.”
CAN IT BE PREVENTED?
Advertisement
Hide AdAdvertisement
Hide AdUnfortunately, there is currently no vaccine to protect against GBS.
In the UK, there is no national screening programme to routinely check all pregnant women to see if they are carrying GBS bacteria.
However, antibiotics can be given to women at increased risk of GBS during labour, and also to babies immediately after birth.
It’s possible to be tested for GBS in late pregnancy.
Sensitive tests designed to detect carriage are available, but rarely within the NHS.
Ask your GP or midwife for details of the ECM (or Enriched Culture Medium) test, which is recognised as the ‘gold standard’ for detecting GBS carriage.