GP shortage in Blackpool is ‘getting worse’
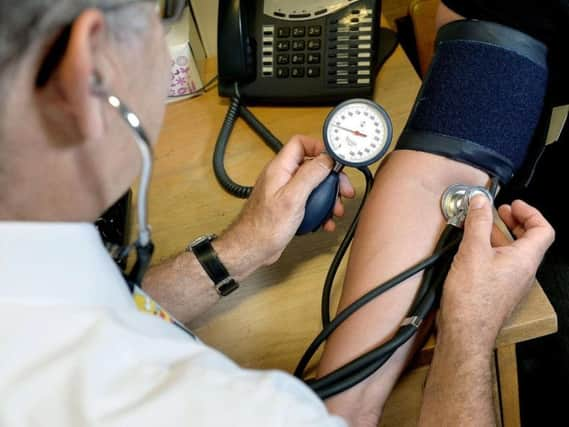

The number of family doctors in Blackpool has dropped in recent years, figures show, and the area has fewer than average GPs per head.
Recent reports show that GP numbers have fallen across the UK over the last five years, with doctors warning that they are seeing more patients than they think is safe.
Advertisement
Hide AdAdvertisement
Hide AdNHS Digital data shows there was the equivalent of 83 full-time GPs in the NHS Blackpool Clinical Commissioning Group in December 2018.
It means there were an estimated 59 GPs for every 100,000 people in the CCG’s area– slightly less than the England average of 62.
It is an increase on the number of GPs when the NHS first published comparable data, in September 2015 – there were 91 in the area at the time.
An analysis by the Nuffield Trust for the BBC found that the number of GPs per 100,000 people across the UK has fallen, from nearly 65 in 2014 to 60 last year – the first sustained fall of this kind since the late 1960s.
Advertisement
Hide AdAdvertisement
Hide AdAnother study by Pulse magazine found that over-tired doctors were sometimes seeing twice as many patients as they should.
It meant that GPs were struggling to be sympathetic to the patients they were seeing during appointments.
The Pulse poll of 1,681 GPs for BBC’s Panorama found that they are working an average 11-hour day, including eight hours of clinical care and three hours of administration.
On average, each GP dealt with 41 patients per day, despite saying 30 was a safe number.
Advertisement
Hide AdAdvertisement
Hide AdOne in 10 dealt with 60 or more patients – double the safe limit.
Professor Helen Stokes-Lampard, chairwoman of the Royal College of GPs, said she is one of those affected by heavy workloads.
She said: “In my own practice recently, I had a 12-hour day and 100 patient contacts. GPs across the UK will tell similar stories.”
Professor Clare Gerada, former chairwoman of the RCGP, said there was a risked tired GPs could make mistakes, and high numbers of patients added to this.
Advertisement
Hide AdAdvertisement
Hide Ad“You could miss a result or misread a letter, or you don’t focus on the right symptom or ask the right question,” she said.
A report in March from the King’s Fund, Nuffield Trust and Health Foundation predicted that GP shortages in England will almost triple to 7,000 by 2023-24.
It said the Government would miss its target to recruit 5,000 more GPs by 2020 and the only way to cope with the growing workload was to put more pharmacists and physiotherapists into GP practices.
Last year, The Gazette reported how retiring doctors were being offered £20,000 a year to stay on in a bid to avoid a shortage, while trainees were offered the same sum in 2016 to start practicing here.
Advertisement
Hide AdAdvertisement
Hide AdDr Amanda Doyle (left), the chief clinical officer at Blackpool CCG and Fylde and Wyre CCG, the groups responsible for organising and paying for residents’ health care, said at the time: “If we can get people here, they stay but the difficulty is getting people to come to Blackpool in the first place.
“All the factors associated with deprivation make the job more of a challenge and harder work for GPs.
“If you are working with a population with much poorer health, then the demands on GPs are much greater and obviously Blackpool has very poor overall health statistics.”
Despite already having one of the lowest rates of GPs relative to the population size, it was also previously revealed how more than one in five of the resort’s 92 family doctors was due to retire in the next five years, leaving an even greater shortfall and potential gaps in care.
Advertisement
Hide AdAdvertisement
Hide AdTwo surgeries have been forced to shut in recent years due to difficulties replacing doctors – and another said it was struggling to maintain its patient boundary due to a shortage of GPs coupled with a rise in patients.